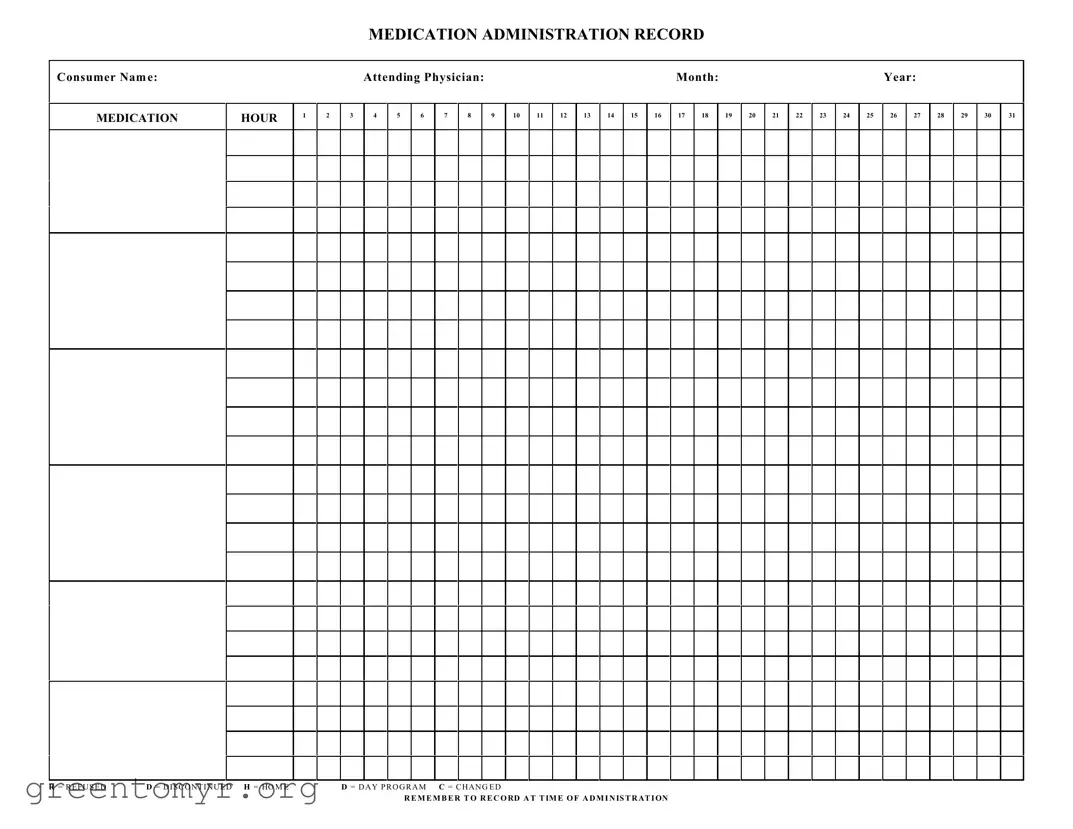
The Medication Administration Record Sheet is an essential tool used in healthcare settings to ensure accurate tracking of medication administration for patients. This form captures vital information, including the consumer's name, the attending physician, and the specific month and year of treatment. It provides a structured way to document the administration of medications throughout the day, with designated hours for each entry. The form includes codes for various situations, such as refusing medication, discontinuing a medication, or changes in the treatment plan, ensuring clarity in communication among healthcare providers. Additionally, the sheet emphasizes the importance of recording medication administration at the exact time it occurs, which is crucial for maintaining patient safety and effective care. By utilizing this form, healthcare professionals can enhance accountability and streamline the medication management process, ultimately contributing to better patient outcomes.