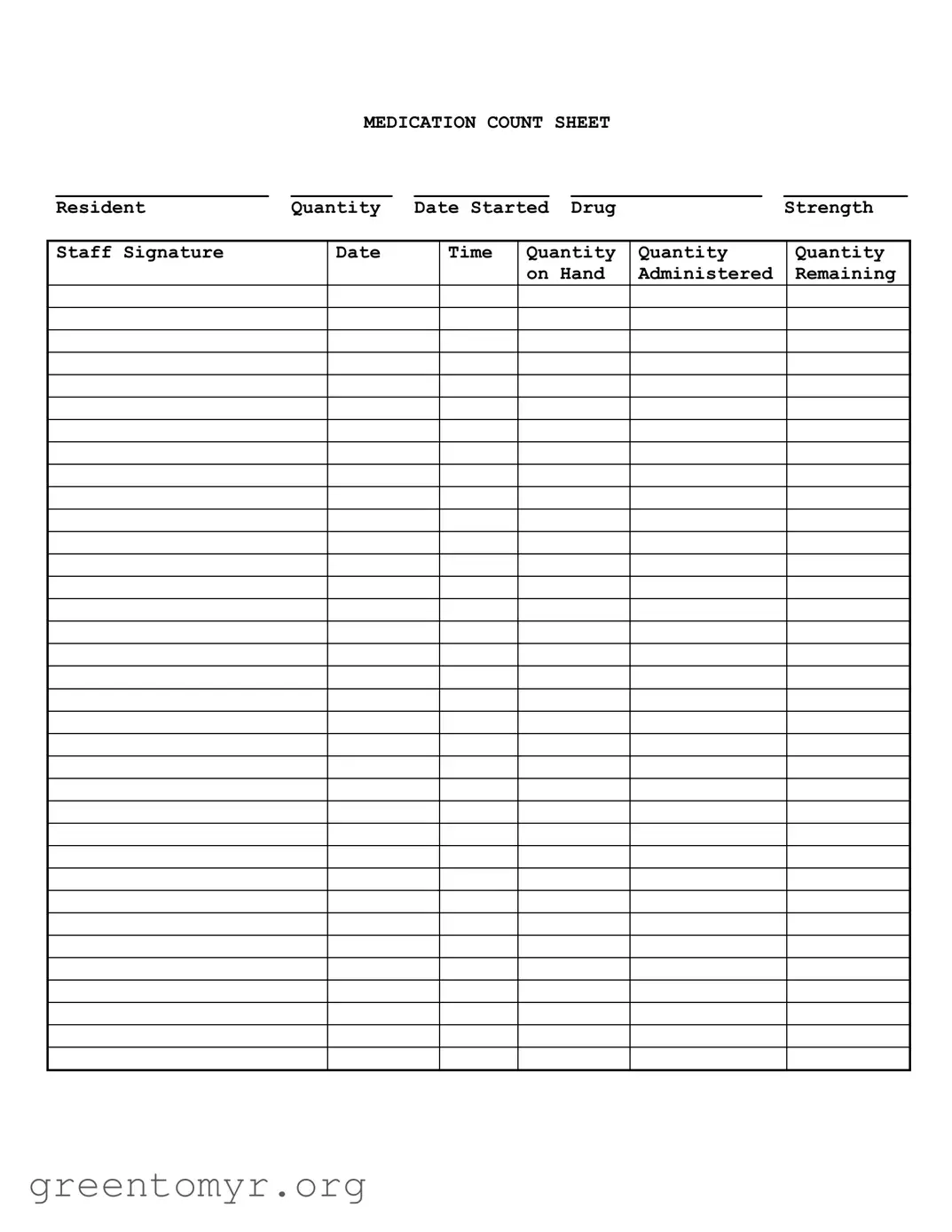
The Medication Count Sheet form is a document used to track the administration of medication to residents in a care facility. It helps ensure that the right amount of medication is given and that there are no discrepancies in the medication inventory.
The form includes several key pieces of information:
-
Resident's name
-
Quantity of medication
-
Date the medication was started
-
Drug strength
-
Staff signature
-
Date and time of administration
-
Quantities administered and remaining
Who is responsible for filling out the Medication Count Sheet?
Staff members who administer medication are responsible for filling out the Medication Count Sheet. This includes nurses, nursing assistants, and any authorized personnel involved in medication management.
How often should the Medication Count Sheet be updated?
The Medication Count Sheet should be updated each time medication is administered. This ensures that the record is accurate and reflects the current status of medication on hand.
Why is it important to keep an accurate count of medication?
Keeping an accurate count of medication is crucial for several reasons:
-
It helps prevent medication errors.
-
It ensures residents receive the correct dosage.
-
It allows for accountability among staff members.
-
It aids in compliance with regulations and standards.
What should be done if there is a discrepancy in the medication count?
If a discrepancy is found, it should be reported immediately to a supervisor. An investigation may be conducted to determine the cause of the discrepancy, and appropriate actions will be taken to resolve the issue.
Can the Medication Count Sheet be used for all types of medications?
Yes, the Medication Count Sheet can be used for various types of medications, including prescription drugs, over-the-counter medications, and controlled substances. Each type of medication should be tracked appropriately to ensure safety.
Is training required for staff to use the Medication Count Sheet?
Yes, staff should receive training on how to properly use the Medication Count Sheet. Understanding the importance of accurate record-keeping and the correct procedures will help maintain the safety and well-being of residents.
Where should the completed Medication Count Sheets be stored?
Completed Medication Count Sheets should be stored in a secure location, such as a locked file cabinet or electronic system. Access should be limited to authorized personnel to protect residents' privacy and ensure compliance with regulations.